Introduction
Physiotherapy in Toronto for Hand Conditions
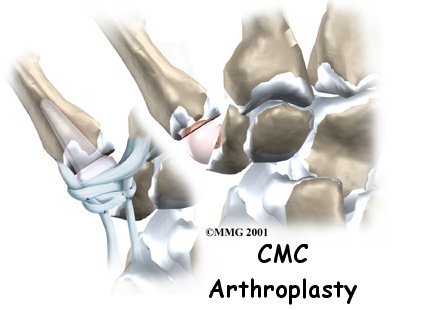
Welcome to Revive Health Centres guide to artificial replacement of the thumb.
If nonsurgical treatments are not successful in easing problems of thumb arthritis, your doctor may recommend replacing the surfaces of the joint. Joint replacement surgery is called arthroplasty.
This guide will help you understand:
- which parts of the thumb are involved
- how surgeons perform this surgery
- what to expect before and after surgery
- Revive Health Centres guide to rehabilitation after surgery
Anatomy
Which parts of the thumb are involved?
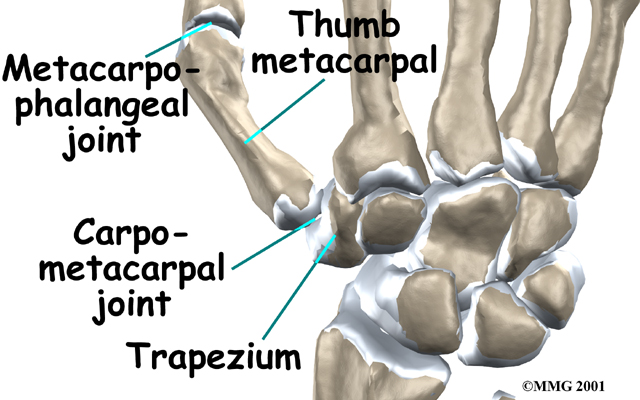
The carpometacarpal joint of the thumb (CMC joint) is where the metacarpal bone of the thumb attaches to the trapezium bone of the wrist. This joint is sometimes referred to as the basal joint of the thumb as it is the joint closest to the bottom of the hand. The CMC is the joint that allows you to move your thumb into your palm, a motion called opposition.


Several ligaments (bands of strong tissue) hold the bones of the joint together. These ligaments join to form the joint capsule of the CMC joint. The joint capsule is a watertight sac around the joint.
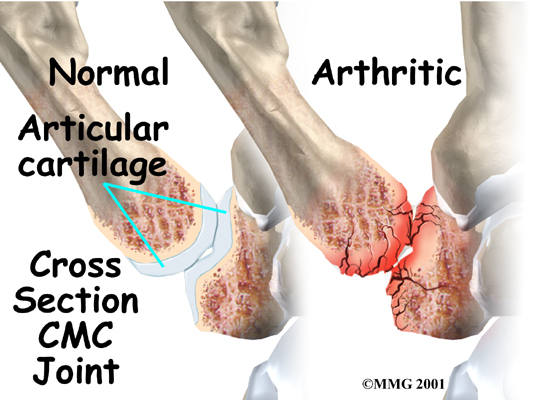
The joint surfaces are covered with a material called articular cartilage. This material is the slick, spongy covering that allows one side of a joint to slide against the other joint surface easily. When this material wears out, the joint develops a type of arthritis called osteoarthritis and becomes painful. Osteoarthritis is the most common form of arthritis occurring at this joint.
Related Document: Revive Health Centres Guide to Hand Anatomy
Hand Anatomy Introduction
Rationale
What does the surgeon hope to achieve?
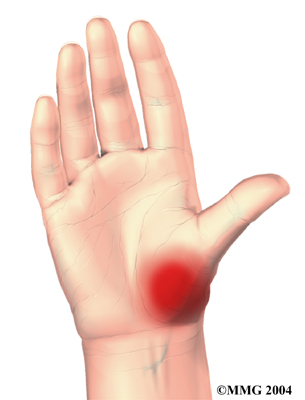
Arthritic joint surfaces can be a source of stiffness, pain, and swelling. The artificial joint is used to replace the damaged joint surfaces so patients can do their activities with less pain. Unlike a fusion surgery that simply binds the joint together, arthroplasty can help take away pain while allowing the thumb joint to retain movement.
Preparation
How should I prepare for surgery?
The decision to proceed with surgery must be made jointly by you and your surgeon. Your physiotherapist may also liaise with your surgeon to confirm the types of therapy techniques trialed and confirm the ineffectiveness of conservative therapy. You need to understand as much about the procedure as possible. Any concerns or questions you have should be brought up to your surgeon.
Once you decide to go ahead with the surgery, you need to take several steps. Your surgeon may suggest a complete physical examination by your regular doctor. This exam helps ensure that you are in the best possible condition to undergo the operation.
A preoperative visit to one of our physiotherapists at Revive Health Centres will also help to prepare you for your surgery. We will start to teach you some of the rehabilitation exercises you will use during your recovery. It is often easier to try these exercises prior to the surgery, when there is no surgical pain and you are feeling well. Your physiotherapist at this time can also help you anticipate any special needs or problems you might have at home, once you are released from the hospital.
On the day of your surgery, you will probably be admitted to the hospital early in the morning. You shouldn't eat or drink anything after midnight the night before. The length of time you spend in the hospital depends on a variety of factors including the ease of the surgery, your body’s reaction to the surgery, as well as any complications that can, but rarely occur.
Surgical Procedure
What happens during surgery?
Before we describe the procedure, let's look first at the artificial thumb joint itself.
The Artificial Thumb Joint
Surgeons have several ways to replace the thumb joint surfaces. One way is to attach the ends of a prosthesis implant into the bones of the thumb joint. A newer method uses a small, marble-shaped implant to form the new joint surfaces. This spherical implant works like a ball bearing to give the joint a smooth arc of movement.
The Operation
The procedure to put in the prosthesis implant takes about two hours to complete. The newer method using the ball implant takes 30 to 60 minutes. Surgery may be done using a general anesthetic, which puts you completely to sleep, or a local anesthetic, which numbs only the hand. With a local anesthetic you may be awake during the surgery, but you won't be able to see the surgery.
Once you have anesthesia, your surgeon will make sure the skin of your hand is free of infection by cleaning the skin with a germ-killing solution.
Prosthesis Implant
In this procedure, an incision is made across the base of the thumb. The soft tissues are spread apart with a retractor. Special care is taken not to damage the nearby nerves going to the thumb. The joint capsule is opened, exposing the CMC joint. The ends of the bones that form the CMC joint surfaces are taken off, forming flat surfaces.
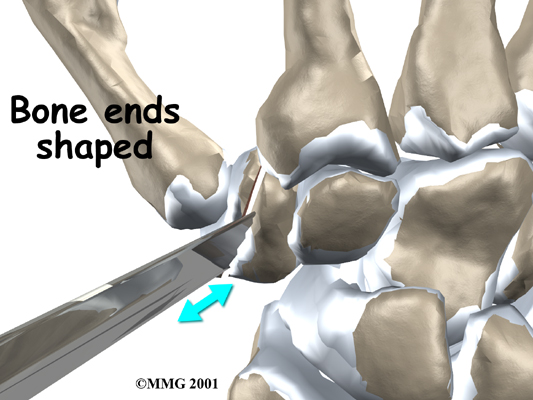
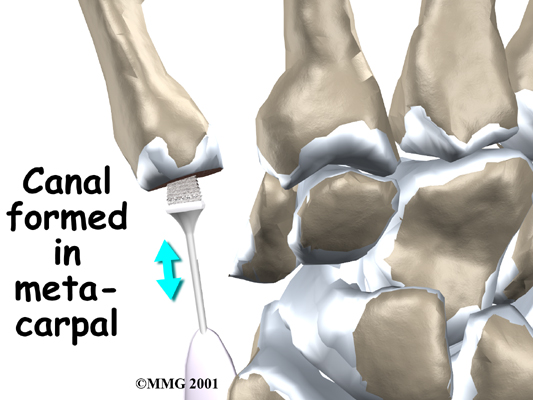
A burr (a small cutting tool) is used to make a canal into the bones that form the thumb joint. The surgeon sizes the stem of the prosthesis to ensure a snug fit into the canal and inserts it. When the new joint is in place, the surgeon wraps the joint with a strip of nearby tendon. This gives the new implant some added protection and stability.
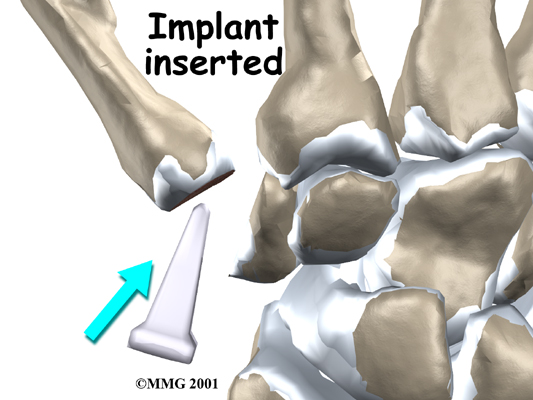
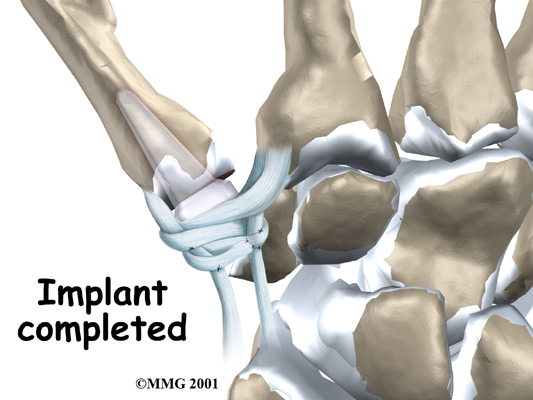
The skin is stitched together and a splint applied.
Spherical Implant
A new method for replacing the thumb joint is to use a spherical implant that looks much like a marble. The surgeon makes a small, one-inch incision at the base of the thumb joint. The ends of the bones that form the CMC joint surfaces are removed, forming flat surfaces.
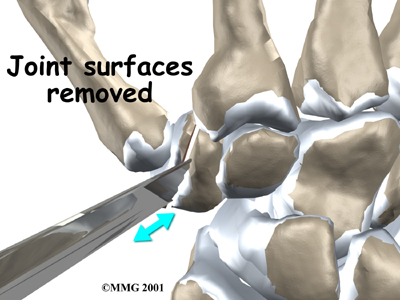
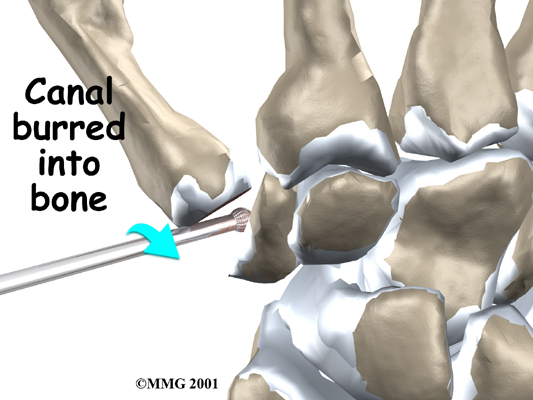
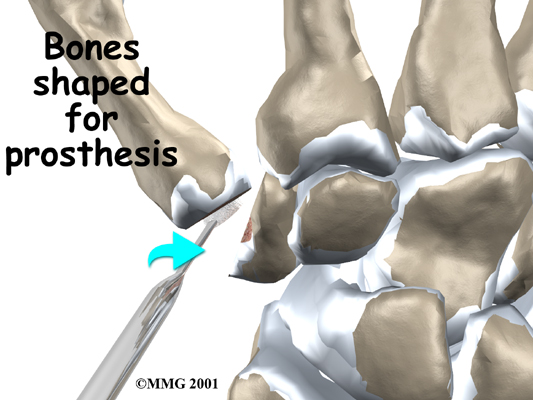
A burr is used to make a small notch, or canal, in the ends of the two bones. The surgeon shapes the notch so the ball-shaped implant will fit snugly in the joint. The implant is placed between the ends of the shaped bones.
The soft tissues are sewn together, and the thumb is splinted and bandaged.
View animation of joint surface removal
View animation of of canal formation
View animation of stem sizing and insertion
View animation of tendon strip addition
After Surgery
What happens after surgery?
After surgery, your thumb will be bandaged with a well-padded dressing and a splint for support. The splint will keep the thumb in a natural position during healing. Your surgeon will want to check your hand within five to seven days. Stitches will be removed after 10 to 14 days, though most of your stitches will be absorbed into your body. You may have some discomfort after surgery. You will be given pain medication to control the discomfort.
You should keep your hand elevated above the level of your heart for several days to avoid swelling and throbbing. Keep it propped up on a stack of pillows when sleeping or sitting up. Ice may also be used at this stage for pain relief.
Complications
What might go wrong?
As with all major surgical procedures, complications can occur. Some of the most common complications with an artificial joint replacement of the thumb are highlighted below:
- reaction to the anesthesia
- infection
- nerve damage
- prosthesis failure
Anesthesia
Problems can arise when the anesthesia given during surgery causes a reaction with other drugs that the patient is taking. In rare cases, a patient may have problems with the anesthesia itself. In addition, anesthesia can affect lung function because the lungs don't expand as well while a person is under anesthesia. Be sure to discuss these risks and your concerns with your anesthesiologist.
Infection
Any operation carries a small risk of infection. Replacing the thumb joint is no different. You will probably be given antibiotics before the operation to reduce the risk of infection. If an infection occurs you will most likely need antibiotics to cure it. You may need additional operations to drain the infection if it involves the area around the hardware. In these cases, the hardware may need to be removed.
Nerve Damage
All of the nerves and blood vessels that go to the thumb travel across, or near, the thumb joint. Since the operation is performed so close to these important structures, it is possible to injure either the nerves or the blood vessels during surgery. The result may be temporary if the nerve injury has come from the nerve being stretched by retractors during the surgery holding them out of the way. It is uncommon to have permanent injury to either the nerves or the blood vessels during this surgery, but it is possible.
Prosthesis Failure
Unfortunately artificial replacement prosthesis can fail. The older silicon-type prosthesis has been shown to break apart and fragment. Most types of prostheses have the potential to displace, or move out of the correct position, causing problems. Most of these problems will require a second operation to remove and replace the prosthesis.
Portions of this document copyright MMG, LLC.


























